Elevate your local knowledge
Sign up for the iNFOnews newsletter today!
Sign up for the iNFOnews newsletter today!
Selecting your primary region ensures you get the stories that matter to you first.
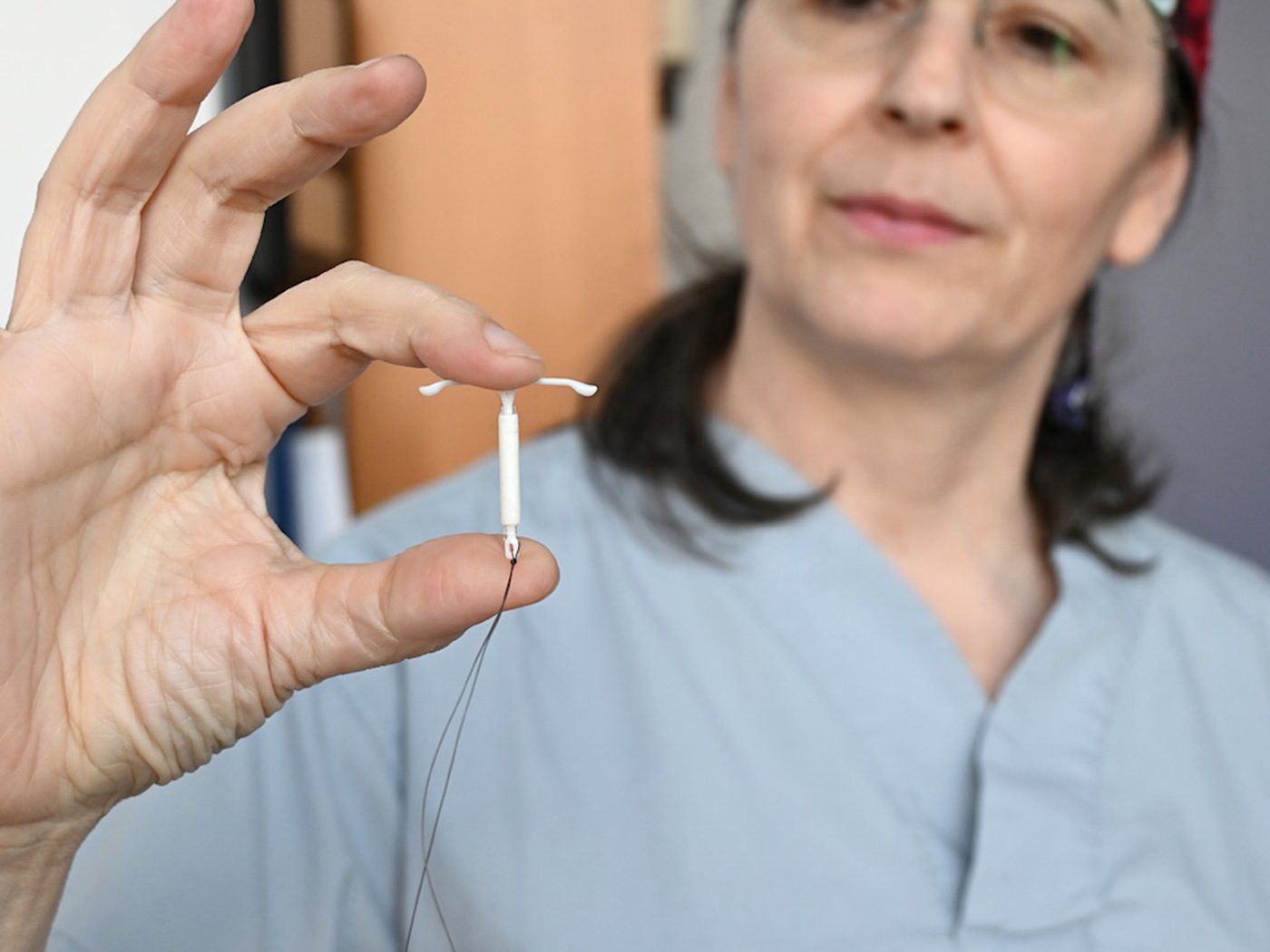
Reproductive justice is being rolled back across the world, making it all the more important to celebrate B.C.’s “wildly successful” free contraceptives program, said Teale Phelps Bondaroff, District of Saanich councillor and co-founder of AccessBC, a society that has been advocating for removing barriers to accessing prescription contraceptives since 2017.
Since the program launched three years ago on April 1, 2023, more than 407,000 free contraceptives have been dispensed, according to the Ministry of Health, with more than half that medication distributed last year alone.
For some patients, one of the biggest concerns used to be about how expensive contraceptives were, said Dr. Renée Hall, medical director of the Willow Reproductive Health Centre in Vancouver and a clinical professor at the University of British Columbia.
“It just so happens that the most effective methods are the most expensive,” she added. In the past, that dissuaded some people who were worried they’d spend hundreds of dollars only to find out the method did not ultimately suit them.
Now, she said, “people have the freedom to choose what works best for them.”
The Ministry of Health says that from April 1, 2023, to Feb. 28, 2026, pharmacies dispensed 232,000 hormonal pills, 105,000 hormonal IUDs, 101,000 emergency contraceptive pills, 17,000 implants, 16,000 copper IUDs, 14,000 hormonal injections and 7,000 vaginal rings as part of the free contraceptives program.
These numbers count medications dispensed rather than patients accessing the medication. So it’s possible IUDs are now the leading contraceptive choice in B.C. as they last for eight to 10 years, while hormonal pills are generally dispensed every three months.
Hall said more British Columbians are using long-acting reversible contraceptives such as IUDs and hormonal implants, which are the most effective at preventing unwanted pregnancy but also have the highest upfront cost. The devices used to cost about $550 and $325, respectively. A hormonal IUD lasts eight years and an implant lasts three.
In the first 15 months of the program an additional 11,365 British Columbians tried out long-acting reversible contraceptives than would have been expected if cost had still been an issue, according to research from UBC’s Contraception and Abortion Research Team. That’s a 49 per cent increase.
The study also found that 10 per cent more reproductive-aged females are using prescription contraceptives now that they are free, compared with before when they had to pay for them.
Health Minister Josie Osborne said the government is “proud” to be the first jurisdiction in Canada offering free prescription contraception.
“Investing in the health of women and gender-diverse people is essential to gender equity,” she said in an emailed statement. “It’s also critical that we support people to take charge of their reproductive health.”
Contraceptives for the rest of Canada
Phelps Bondaroff said free contraceptives appeal to the entire political spectrum because they save the government money — contraceptives are cheaper than abortions — and reduce the number of elective abortions by helping prevent unwanted pregnancies.
The Health Ministry said it has distributed at least 101,000 free emergency contraceptive pills, such as Plan B, since the program started, which is 101,000 potential elective abortions the government didn’t need to provide, Phelps Bondaroff said.
AccessBC celebrated when B.C. introduced free contraceptives in 2023, but the fight was far from over, he said.
Since then it has been advocating for the province to offer more contraceptive options and working with sister campaigns in different provinces and territories to help them advocate for their own provincial program, he said.
In 2025 Manitoba, B.C., P.E.I. and the Yukon signed on to then-prime minister Justin Trudeau’s national pharmacare plan, which offered universal coverage of contraception and diabetes medications. B.C. used this deal to get the federal government to also cover menopausal hormone therapy, which began March 1.
However, Phelps Bondaroff said, since coming to power Prime Minister Mark Carney has “flip-flopped” on pharmacare, and it isn’t clear if the federal Liberals want to sign more provinces and territories onto the plan. That is creating unequal access to this “life-changing” medication, which is not allowed under the Canada Health Act, he added.
Access to contraceptives can be life-changing because it allows people to choose if and when they want to be parents, which benefits them and their potential children.
Phelps Bondaroff said AccessBC has calculated that 62 per cent of the federal funding envelope has already been allocated to the jurisdictions already signed up, which means it’s unclear how the program could expand to cover larger jurisdictions such as Quebec and Ontario. It calculated this by adding up how much funding each province and territory received through the national pharmacare deal. B.C. was allocated $670 million over four years, Manitoba $219 million over four years, P.E.I. $30 million over four years, and Yukon $9.5 million over four years. The 2024 federal budget says pharmacare would be financed by a $1.5-billion investment over five years, which means 62 per cent of that $1.5 billion is already spoken for.
Back in B.C., AccessBC has launched a new campaign working to improve pain management for IUD insertions.
The Not Just a Pinch campaign was launched in December and is asking the province to increase access to numbing and cervical blocks, which are already covered by the Medical Services Plan, and to offer methoxyflurane, better known by the brand name Penthrox, during IUD insertions.
Health Canada approved the use of methoxyflurane in 2022, but the drug has been used in Australia and New Zealand since the 1970s for short-term pain management.
Family planning specialist Hall said she has been advocating for improved physician education about pain management for years and has recently been seeing some improvement as she meets more students who are thinking about and have questions about pain management.
What contraceptives to use and the benefits and drawbacks of each method should always be a conversation between a patient and their clinician, she said, adding that potential pain and pain management should be part of that discussion.
That conversation can also provide a time for clinicians to identify and respond to any misinformation a patient might have, she said.
She said a lot of patients in their 20s are getting misinformation about hormonal birth control from social media, where influencers say that “all hormones are bad for you.”
That’s not true, she said. But it is true that all medications have some risk, which is why a patient should always talk with a clinician about what birth control is right for them. She added that the risks always need to be balanced against the risk of pregnancy.
The most effective birth control option out there is for a male partner to get a vasectomy, which is fully covered by the Medical Services Plan in B.C. and is offered at the Willow Reproductive Health Centre, Hall said. In some cases this procedure can be reversed, but in general it is considered permanent, Hall added.
In July B.C. also launched its in vitro fertilization program, where each patient could have access to one-time funding of up to $19,000 for a single standard IVF cycle. The Health Ministry says more than 1,600 individuals and couples have been approved for funding through the IVF program, with more applications in progress.
News from © iNFOnews.ca, . All rights reserved.
This material may not be published, broadcast, rewritten or redistributed.

This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
Want to share your thoughts, add context, or connect with others in your community?
You must be logged in to post a comment.